Flat Feet – Posterior Tibial Tendon Dysfunction
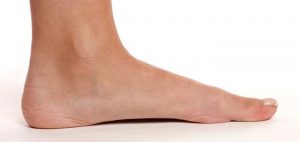
Flat feet, also known as a decreased or fallen arches or flat feet, can be a source of significant pain and debilitation. Pain can interfere with walking, exercise, and performing normal activities of daily living. Although flat feet often present with similar symptoms, the term flat feet is an over-arching term that represents various causes of a decreased arch with restricted foot motion and foot pain. After determining the cause of the flat foot, a more focused treatment plan can be developed.
A thorough history and physical examination is the first part of evaluating flat feet. An x-ray is often taken to rule-out any specific osseous (bony) causes of flat feet. It is important to determine if the foot is flexible, meaning that there is motion in the back of the foot, or if the foot is rigid, meaning that there is limited or no motion in the back of the foot. It is also important to evaluate the strength and integrity of the posterior tibial tendon, one of the strongest tendons of the foot and ankle that help to maintain the arch.
Advanced imaging, such as an MRI or CT scan, may also be indicated to evaluate the integrity of the posterior tibial tendon. These scans can also help to rule-out coalitions, which are abnormal connections between bones that normally do not connect, since this can restrict motion and cause a flat foot.
Symptoms of Flat Feet
- Pain or irritation of the inner foot and ankle
- Pain that is worse with activity (running, walking, high-impact activities)
- Pain on the outer ankle of the affected extremity
- Swelling, redness, or burning to the inner foot and ankle
- Increase in foot size or shoe size as the foot flattens out and elongates
- Limited flexibility and range-of-motion of the affected foot
- Decreased strength of the affected foot and ankle
Non-Surgical Treatment of Tibial Tendon Dysfunction
There are a variety of treatment options for flatfeet. Treatment options depend upon the severity of your flatfeet and other factors. A number of non-surgical measures can be undertaken:
- Changes in shoe gear: use more supportive shoe gear that have structure and rigidity
- Avoid shoes with high heels
- Orthotic devices and bracing: a custom orthotic device placed in your shoe may help control the muscle/tendon imbalance and provide biomechanical support to the foot and ankle
- Injection therapy: corticosteroid injections are sometimes used to ease pain and inflammation
- Medications: oral nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen and naproxen, may be recommended to reduce pain and inflammation
- Splinting/strapping: splints or small straps may be applied to help with support and structure
- Ice therapy
- Physical therapy
Surgical Treatment
- Tenosynovectomy: removing the inflamed and degenerative portion of the tendon to remove pathologic tissue and reduce pain, which can sometimes be performed via a minimally-invasive technique
- Tendon repair or tendon transfer: if there is a tear in the tendon, the tear will need to be repaired with sutures, however, if the tear is too substantial then the tendon may have to be sutured to an adjacent tendon to increase the strength and stability of the foot and ankle
- Osteotomy (cutting and shifting bones): there is often bony instability and misalignment that contributes to excessive forces on the tendon and earlier dysfunction and breakdown, thus realigning the bones with internal hardware can provide a more supportive bony structure for the tendon to work around
- Fusion of joint(s): if the symptoms are long-standing and there are degenerative arthritic changes to the joints in the back of the foot, a fusion (or joining of two bones) may be necessary to reduce pain and realign the structure of the foot
Recovery from surgery varies. Post-operative protocol will include ambulation in a walking boot at one of the spectrum to a period of immobilization and non-weight bearing of the affected extremity on the other end of the spectrum. Recovery will also include directed physical therapy to regain strength, balance, and range of motion.
